Disclaimer: A suspected finding does not always lead to a CUP diagnosis. Check with your healthcare team if you're unsure whether this information is relevant to you.
Cancer of Unknown Primary (CUP) is where cancer has been found in the body, but the primary site of origin (i.e., where the cancer started) remains unknown, despite comprehensive testing and specialist review.
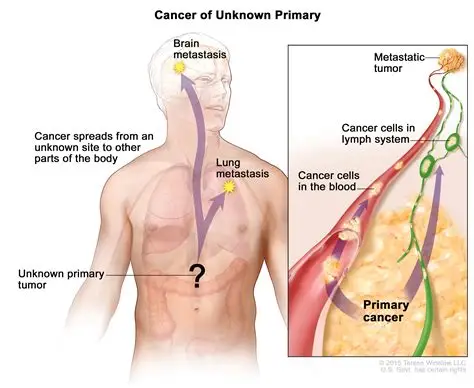
CUP can be a suspected diagnosis, or a confirmed diagnosis:
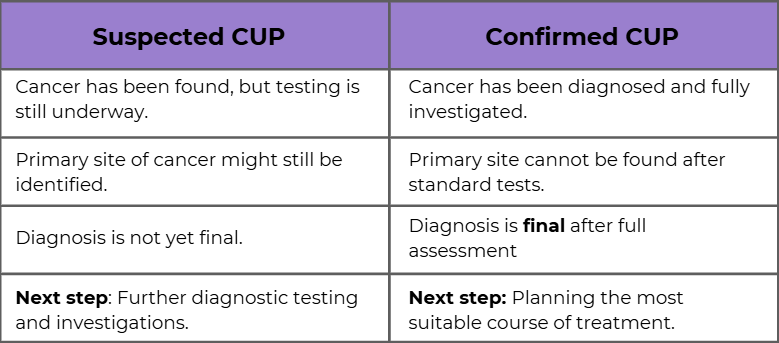
Suspected CUP
A “suspected CUP” diagnosis means cancer has been found in the body, but the place where it began is not yet known. If you have a suspected CUP diagnosis, your healthcare team will be conducting more tests to try to understand the type of cancer you have, and where it may have started.
Confirmed CUP
A “confirmed CUP” diagnosis means that cancer has been diagnosed, and despite all the recommended tests, the place where the cancer began cannot be found. Even though the primary site is unknown, your healthcare team can still provide treatment based on the cancer’s features and how it affects your body.
There are several reasons why your doctors might not be able to find the primary cancer.
These include:
Your doctor may have other reasons to explain why the primary cancer cannot be found. Even if the primary cancer cannot be found, treatment options may still be available based on the most likely cancer diagnosis.
Like a detective, doctors will try to learn as much as possible about your medical history, your risk factors for cancer, symptoms,and the spread of cancer. The type of CUP is determined by doctors trying to identify or strongly suspect where the (primary) cancer started in the body. The location of the primary cancer helps to determine the most appropriate treatment options, as some cancer types are predictable in their disease pattern.
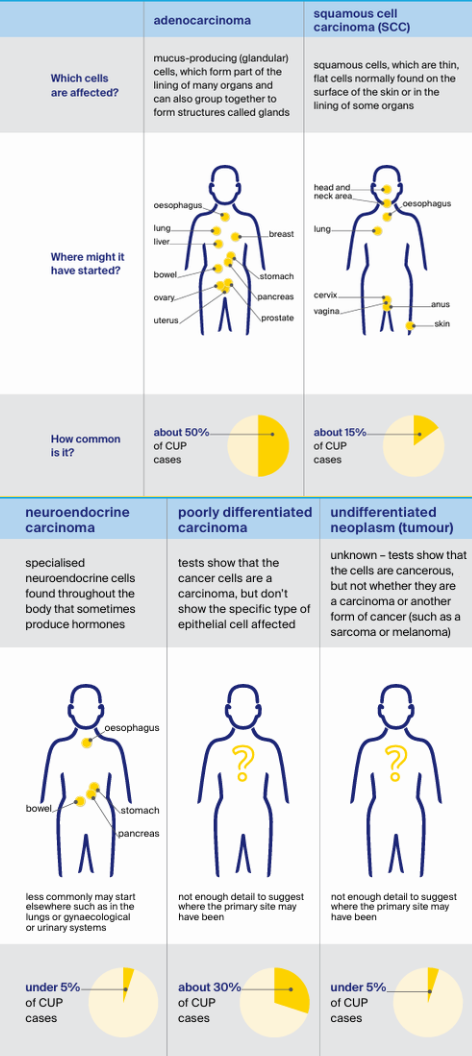
Most cancers originate from epithelial cells, which are found in the skin and the outer lining of internal organs. More specifically,CUP types are:
View or download The Cancer Council pamphlet on “what to expect during each stage of treatment and beyond” for CUP patients.
Doctors conduct a range of tests to determine the size of the tumour, if it has grown over time, and if it has spread to other parts of the body. This is called staging and it helps inform doctors on the best treatment plan for their patients. Each cancer has slightly different staging systems. For most types of cancer, there are 4 stages:
There is NO staging system for CUP as doctors do not know where the primary cancer is. However, as the cancer has spread, CUP is considered to be a Stage 4 or an advanced cancer. Therefore, the goal of treatment in many cases may not be to eliminate or remove the cancer, but to focus on slowing down the spread of cancer, controlling symptoms and maintaining the best possible quality of life. Patients with only localised areas of CUP cancer may be suitable for local treatment with the intent of completing removing the cancer, either with surgery or radiotherapy.
CUP is mostly detected after the cancer has already spread to other parts of your body. Whilst treatment may be able to control cancer and improve your symptoms, it is unlikely to cure it. Your doctor will discuss all the treatment options that are available to you. Options will depend on many factors, including the location(s) of your cancer, your overall health, and your wishes and goals of care.
Sometimes a multidisciplinary team (a group of medical professionals from different specialties) may meet to discuss your case and which option should be recommended for your case. There are various treatment options available for CUP. The most common treatment for CUP is chemotherapy. You may also have other drug therapies such as hormone therapy, targeted therapy, immunotherapy, or other treatments such as radiation therapy or surgery. Different types of treatment may be combined. It is possible that treatment may not cure you from cancer but make you feel better and also help you live longer.
The CUPiD study is exploring how advanced genomic testing can help identify the possible origin of cancers that do not have a known primary site. This testing is done on a biopsy sample - usually one that has already been taken. In some cases, a new biopsy may be needed if the original sample is not suitable. Finding a potential primary cancer site can help your doctor tailor treatment more specifically to your needs. Please note: this study is for testing purposes only and does not provide treatment.
Who Can Take Part?
You may be eligible to participate in the CUPiD study if you:
✅ Have a suspected or confirmed diagnosis of CUP
✅ Are not currently receiving treatment through this study - it is for testing only
✅ Have a biopsy sample available (usually previously taken).
In some cases, a new biopsy may be needed if the original sample is not suitable.
Who Cannot Take Part?
You may not be eligible if:
❌ Your cancer has spread from a known primary site.
❌ You have had previous test results that clearly point to a specific cancer type or origin.
Where Is the Study Available?
This study is currently recruiting at the following hospitals:
· Royal Adelaide Hospital (SA)
· Flinders Medical Centre (SA)
· Queen Elizabeth Hospital (SA)
· Lyell McEwin Hospital (SA)
· Mount Gambier and Districts Health Service (SA)
· Royal Darwin Hospital (NT)
More Information:
If you're considering joining a clinical trial, please speak with your treating doctor. They can help determine whether a trial is appropriate for you and whether you meet the eligibility criteria.
The FAPI-CUP study is testing a specialised type of PET scan, called the 68Ga-FAPI-PET-CT scan, to help find out where a cancer may have started. This scan is different from the standard FDG-PET scan and may be more effective at detecting certain tumour types - some of which are linked to CUP.
Who Can Take Part?
You may be eligible if you:
✅ Have a confirmed diagnosis of CUP
✅ Have completed your diagnostic workup (standard tests to try to find the cancer’s origin)
✅ Are well enough to undergo a PET scan (your doctor will confirm this)
✅ Are 18 years or older
Who Cannot Take Part?
You may not be eligible if you have:
❌ Already started your line of cancer treatment
❌ Had major surgery in the last 6 weeks
❌ A medical condition that could affect the scan or your safety
❌ A cancer diagnosis in the last 3 years (some exceptions apply)
❌ An allergic reaction to PET scan tracers (such as 18F or 68Ga)
Where Is the Study Available?
This study is currently recruiting at:
More Information:
FAPI-CUP Study | Clinical Trials Australia
If you're considering joining a clinical trial, please speak with your treating doctor. They can help determine whether a trial is appropriate for you and whether you meet the eligibility criteria.
There are many useful online resources about CUP, however, they can become overwhelming. The resources below are endorsed by our CUP experts as the best sources of support and reliable information.
Understanding Cancer of Unknown Primary PDF Booklet | Cancer Council
Cancer Council provides a downloadable booklet providing information on CUP for patients, carers and others that are affected. This includes explaining CUP, the diagnostic process, treatment, care after treatment and support and services. This booklet is often used as a reference by doctors to explain CUP.
Optimal Care for Cancer of Unknown Primary | Cancer Council
The CUP Optimal Care Pathway provides an overview of what to expect for patient care throughout the journey of a CUP diagnosis, including investigations, treatment and living with cancer.
Our Mob and Cancer provide information and support specifically for Aboriginal and Torres Strait Islander People affected by cancer. This page provides an overview of cancer of unknown primary and its treatment, alongside other resources that might be useful during your care.
The websites listed below are international resources providing detailed information about CUP for patients and carers, including the diagnosis, treatment and management of CUP. While the sections on support services are country-specific, you might find it useful to read other sources of relevant information.
Jo's Friends | UK
Jo’s Friends provides detailed information about CUP for a broad audience including patients, carers, researchers and clinicians. It was established in the UK to raise awareness about CUP and provide support to CUP patients and carers.
Cancer of Unknown Primary | Cancer Research UK
Cancer Research UK provides detailed information about CUP, including diagnosis, treatment and management. There is a section about coping with a CUP diagnosis.
Cancer of Unknown Primary (CUP) | Macmillan Cancer Support (UK)
Macmillan Cancer Support resource provides information about CUP diagnosis with links to relevant tests and procedures.
Cancer of Unknown Primary | American Cancer Society
American Cancer Society provides an “easy reading” section on CUP and an in-depth version. There are downloadable PDFs.
Cancer of Unknown Primary | World CUP Awareness
World Cup Alliance advocate for the interests of people impacted by Cancer of Unknown Primary. They are dedicated to improving the quality of care and life by providing information and support for patients.

Living with CUP can be quite challenging, including during the recovery period after treatment. You might continue to experience some side effects after you have finished treatment, such as fatigue, or there might be some side effects that show up after treatment. These are sometimes called “late effects” and they can appear months after treatment has concluded. During your follow-up care, your doctor and healthcare team will help you manage these side effects while monitoring your health. See below for more information regarding your follow-up care.
A CUP diagnosis can continue to have an impact on your emotional and mental health, even after treatment. This can be due to poor understanding of your diagnosis, a sense of frustration with your doctors who are not able to provide you with answers and a general uncertainty about CUP. Depressive symptoms are also more likely to appear in CUP patients. It is important to stay connected to your support system, which can include family and friends, mental health professionals and support groups. They will be able to provide practical and emotional support. Speak to your doctor about how you are feeling as they can refer you to a mental health professional.
To support your recovery, try to maintain a healthy lifestyle. Focus on consuming a balanced diet from the five food groups (wholegrains, meat or alternatives, dairy or alternatives, fruit and vegetables). This will ensure you maintain your weight and provide you with plenty of nutrients and energy to support your recovery. Completing regular physical activity will also help you maintain your weight and rebuild your muscle strength. These habits can support your immune system and overall wellbeing.

Follow-up care allows your doctor and healthcare team to monitor your health after treatment has finished. This includes managing any side effects that you experienced after treatment and checking for recurrence (cancer returning), so it can be treated or managed quickly. Follow-up care is vital for managing a CUP diagnosis so changes in your health can be managed as soon as possible. This is also a good chance to discuss with your doctor anything you are concerned about.
Follow-up care often includes routine tests, such as blood tests and scans every few months if you are well enough. This can be referred to as active surveillance. You can talk to your doctor about the specific tests that are best for you. For those who are involved in a clinical trial, other tests may be included in your care as well.
Your follow-up care will be based on how well CUP responded to treatment. Any tests your doctor recommends and who is involved in your care will also be dependent on your individual circumstances. You might be referred to other specialists such as a social worker, dietitian or mental health professionals to support your overall care. You might also be referred to a palliative care team to manage any side effects or symptoms you are experiencing.
Depending on your situation, you may be advised to continue cancer screening that is recommended for the general population, which can include screening for colon, breast, prostate and skin cancer. If there is a family history of cancer or gene testing has raised suspicion of a specific mutation for cancer, genetic counselling and testing might be offered. This can also lead to additional screening if it is confirmed.
If you notice any unexplained or unintentional weight loss, persistent pain or any other changes in your health that concern you, speak to your doctor.
Watch and listen to CUP patients and carers share their stories and personal experiences to provide support and inspiration for those affected by CUP.
Clinicians also share their expert insights about CUP to help patients, carers and other health professionals understand this diagnosis.
Here are the links to other information pages to learn more about different aspects of the diagnostic journey. You may also use the quick links on the right side of the page to navigate.

Investigations for a suspected cancer can lead to various diagnostic outcomes. To learn more about the different types of diagnosis, click here.




