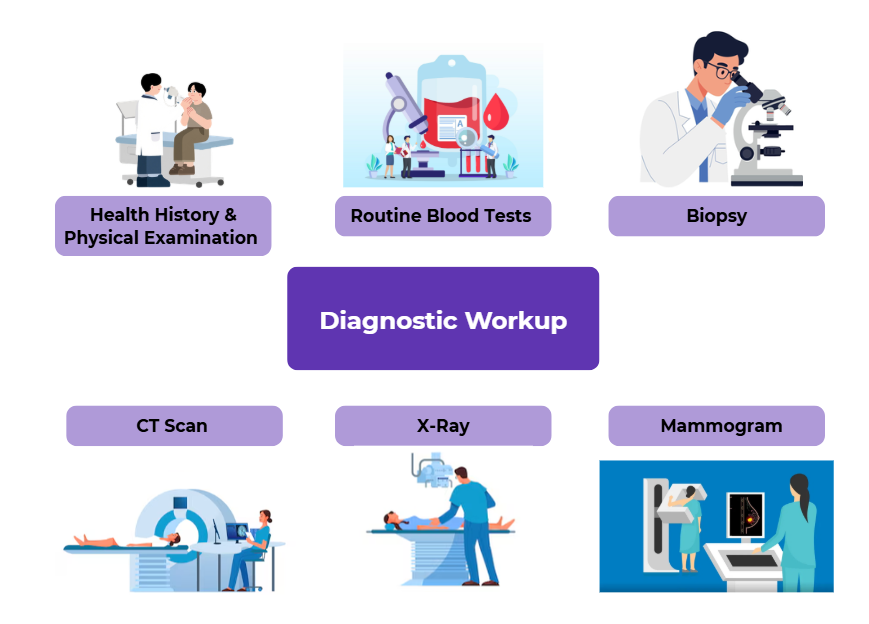
This section provides information on the types of tests and investigations that may be required for you to receive a diagnosis. When deciding what tests to refer you for, your healthcare team will refer to a diagnostic guideline, known as a diagnostic workup. The purpose of this workup is to try to determine whether a cancer is present, where it started, and how far it may have spread as quickly as possible, avoiding unnecessary and repetitive testing. The workup is then used to guide your clinicians next steps, including referral to specialists or further testing if needed.
Typically, a minimum diagnostic workup will include:
Your doctor will conduct a physical examination of your body. Your doctor will pay particular attention to the areas of your body where you are experiencing symptoms, which will be guiding the exam. This can include looking for lumps on your body, feeling for swollen lymph nodes or anything that might be unusual.
Your doctor will also have a discussion with you about your health history and your family history. This can include:
Blood tests check the number of white blood cells, red blood cells and platelets in your blood. This is usually referred to as a complete blood count (CBC), full blood count (FBC), or full blood examination (FBE). They can also check the health of your kidneys and your liver.
How it works:
X-rays deliver low-energy beams of radiation to create images of parts of the body to produce the pictures. X-ray beams are absorbed differently by structures in the body, such as bones that absorb radiation easily (appearing white in the picture) or soft tissues like organs that don’t absorb radiation as easily and will appear gray.
How long:
10-30 minutes.
What happens:
Some x-rays use dye (contrast) to improve the image and make certain structures easier to see. Depending on what part of the body is being x-rayed, you might be asked to lie, sit or stand. You will hold still in front of or on a machine while the images are taken.
Special notes:
The procedure is painless with only a small dose of radiation. The contrast dye is generally very safe and reactions are uncommon; however, people with diabetes and kidney disease should inform their doctor as they will have a slightly greater risk of reaction.
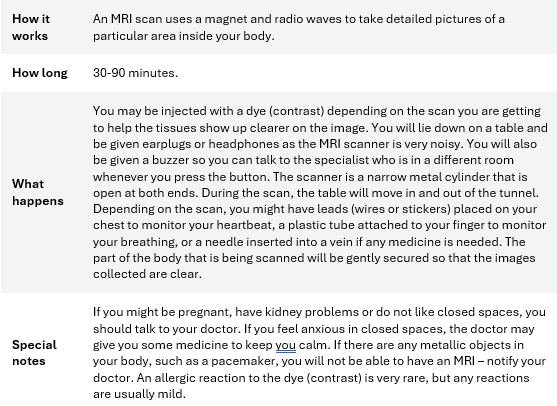
How it works
A CT scan uses x-ray beams and a computer to create detailed pictures of the inside of the body. The scanner is large and shaped like a doughnut. CT scans will provide more detail than an x-ray as it takes dozens to hundreds of images of your body. This provides a clearer image of soft tissues in the body, which don’t always show up on a regular x-ray, and also shows organs and other structures that overlap or are hidden.
How long
30-60 minutes (mostly due to preparation).
What happens
Before the scan, you may be given a drink or injected with a dye (contrast) to highlight certain structures in your body. This will make the images clearer. You will usually lie still on a table that moves into the scanner. It is important to lie still as movement could cause blurry or less clear images.
Special notes
The procedure is painless; however, the dye can make you feel hot or flushed and leave a bitter taste in your mouth. There is a small risk of having an allergy-like reaction to the dye, such as a rash, itchiness, nausea, sweating or difficulty breathing. If you know that you have an allergy to the dye or contrast, or if you are diabetic or have some known kidney issue, inform your doctor. You should also notify your doctor if you are pregnant (or think you may be) as CT scans use slightly higher levels of radiation than x-rays.
How it works
An x-ray machine that is designed only for mammograms will use low-dose x-ray beams to create an image of the inside of the breast.
How long
10-30 minutes.
What happens
You will stand in front of an x-ray machine that is specially designed for mammograms. Your breast is placed between two x-ray plates, one at a time, which will press together firmly to spread the tissue so a clear image can be taken. This also prevents movement so the image does not become blurred. Usually two different views are taken of each breast. During the brief period when you are exposed to the x-ray beams, you will be asked to stand still and hold your breath.
Special notes
The procedure can be uncomfortable when the x-ray plates are pressed together. If the discomfort becomes too much, notify the technologist (the person performing the procedure). You should notify your doctor if you are pregnant (or believe you are) or breastfeeding.
A biopsy is a procedure to obtain a small amount of tissue for testing, with the overall purpose of identifying the type of cancer and, if possible, the original location of the cancer. This may help to guide your doctors in making a diagnosis and choosing the best treatment option. However, if the cancer is too hard to reach or if you are too unwell for the procedure, your doctor might decide against performing a biopsy.
There are multiple ways to obtain a tissue sample and the method used will depend on the type of mass and location in the body. Depending on the method, you will have local anaesthesia to numb the area or general anaesthesia to make you unconscious during the procedure.
Role of the Pathologist in getting a diagnosis
After you have a biopsy, it will be sent to a laboratory for testing. The sample of tissue will be looked at under a microscope by a specialist doctor called a pathologist. A pathologist is a doctor specialising in the diagnosis of disease based on examination of tissues and fluids removed from the body. Upon examination, the pathologist determines if the tissue sample contains normal, pre-cancerous or cancerous cells and then writes a report on their findings (pathology report).
Watch and listen to a pathologist explain their role in getting a diagnosis:
The pathologist will try and identify the type of cancer present in the biopsy, determine the original location of the cancer, and provide information that may help to identify the best treatment option. This helps to guide the clinical team in making a diagnosis and choosing the best treatment. Cancer changes the appearance of healthy cells, making them look abnormal. Pathologists can also identify which cells do not belong in the tissue or organ that it has spread to and are able to identify it as a secondary cancer. Sometimes, the primary cancer is not easily recognisable. These cells may have become so abnormal that it is difficult to identify where they came from. These cells are called poorly differentiated or undifferentiated. Further testing may be required, such as immunohistochemistry, where the pathologist uses special stains to locate specific proteins that are linked to known cancer types (e.g., adenocarcinoma, squamous cell carcinoma).
Watch and listen to a pathologist explain their role in interpreting biopsy results:
Your clinician may request further testing to reach a diagnosis. Some tests that you may be referred for are outlined below:
Urine tests assess the health of the kidneys and the bladder by looking for any blood or abnormal cells that are present. In some cases, blood and urine tests may also be able to focus on a protein that could help diagnose a blood cancer called myeloma.
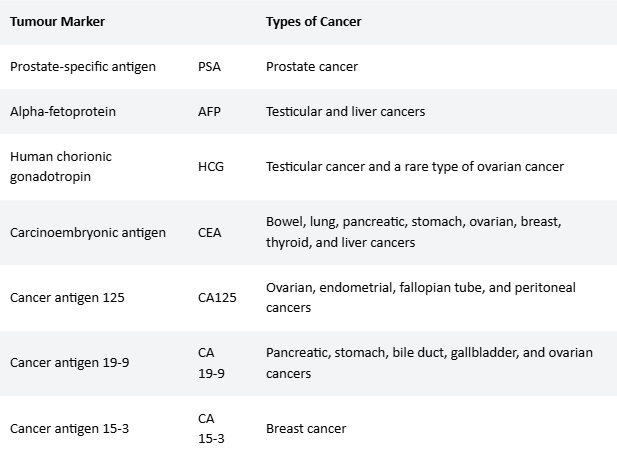
Tumour markers might suggest certain types of cancer. Cancers can release certain chemicals into the body called tumour markers that can be produced by one or several types of cancer. High levels can be found in the blood, urine or other bodily fluids of some people with cancer.
PET Scan (Positron emission tomography scan)
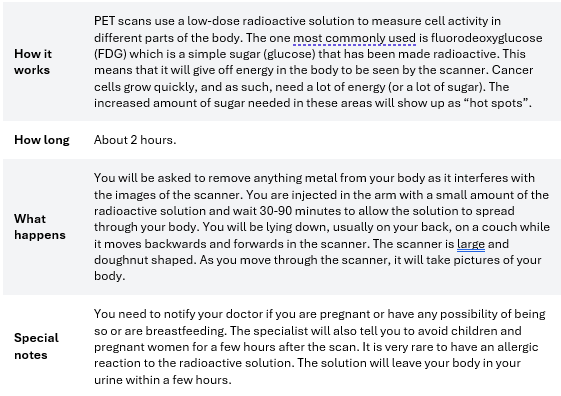
PET- CT Scan
Bone Scan

MRI Scan (Magnetic resonance imaging)
Genomic testing may be available through clinical trials or other options if you’re eligible. If you have questions about genomic testing, please speak to your healthcare team.
Here are the links to other information pages to learn more. You may also use the quick links on the right side of the page to navigate.

Investigations for a suspected cancer can lead to various diagnostic outcomes. To learn more about the different types of diagnosis, click here.




